Endotracheal tubes are a mainstay of hospital care, as they ensure a patient’s airway is clear when they can’t breathe on their own. However, keeping a foreign object inserted in this highly sensitive part of the anatomy comes is not without risk, such as the possibility of infection, inflammation and a condition known as subglottic stenosis, in which scar tissue narrows the airway.
Broad-spectrum antibiotics are one way to mitigate these risks, but come with risks of their own, including harming beneficial bacteria and contributing to antibiotic resistance.
With this conundrum in mind, Riccardo Gottardi, Assistant Professor of Pediatrics at the Children’s Hospital of Philadelphia (CHOP) and of Bioengineering at Penn Engineering, along with Bioengineering graduate students and lab members Matthew Aronson and Paul Gehret, are developing endotracheal tubes that can provide a more targeted antimicrobial defense.
In a proof-of-concept study published in the journal The Laryngoscope, the team showed how a different type of antimicrobial agent could be incorporated into the tubes’ polymer coating, as well as preliminary results suggesting these devices would better preserve a patient’s microbiome.
Instead, the investigators explored the use of antimicrobial peptides (AMPs), which are small proteins that destabilize bacterial membranes, causing bacterial cells to fall apart and die. This mechanism of action allows them to target specific bacteria and makes them unlikely to promote antimicrobial resistance. Prior studies have shown that it is possible to coat endotracheal tubes with conventional antibiotics, so the research team investigated the possibility of incorporating AMPs into polymer-coated tubes to inhibit bacterial growth and modulate the upper-airway microbiome.
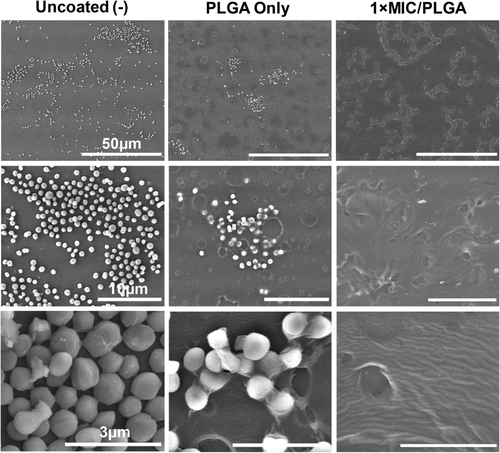
The researchers, led by Matthew Aronson, a graduate student in Penn Engineering’s Department of Bioengineering, tested their theory by creating a polymer coating that would release Lasioglossin-III, an AMP with broad-spectrum antibacterial activity. They found that Lasio released from coated endotracheal tubes, reached the expected effective concentration rapidly and continued to release at the same concentration for a week, which is the typical timeframe that an endotracheal is used before being changed. The investigators also tested their drug-eluting tube against airway microbes, including S. epidermidis, S. pneumoniae, and human microbiome samples and observed significant antibacterial activity, as well as prevention of bacterial adherence to the tube.
Read “CHOP Researchers Develop Coating for Endotracheal Tubes that Releases Antimicrobial Peptides” at CHOP News.
